Chronic diseases are non-communicable illnesses that are prolonged in duration, do not resolve spontaneously, and are rarely cured completely. A diagnosis of a chronic health condition can lead to feelings of shock, anger, grief, loss and sadness are common. These feelings usually pass with time, however, if they cause ongoing stress, you may be at greater risk of developing depression and anxiety. Sufferers find themselves in a double bind where their depression and anxiety is brought on by the deterioration of their physical health. But research shows that depression and anxiety can itself affect your symptoms and physical health adversely. Both mental health disorders and chronic diseases are common and disabling but together they pack a punch!
If you have a chronic physical illness, anxiety or depression can make living with the condition even more difficult. It can make it harder for you to find the energy to eat healthily, exercise or take medication regularly. Depression is more debilitating than the feelings of frustration or disappointment at having a chronic health condition. You may lose enjoyment, as well as the other changes. Some chronic physical illnesses, such as chronic pain, can be largely invisible so that you can feel misunderstood and stigmatised by co-workers, friends, family and even the medical profession. Having a chronic physical illness can also make it seem like an effort to connect with family members and friends. This can make you feel isolated and make it harder to recover from anxiety or depression.
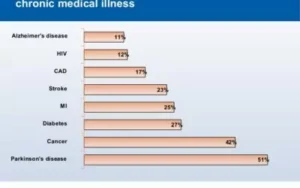
Depression is common among people who have chronic illnesses such as the following:
- Cancer
- Coronary heart disease
- Diabetes
- Epilepsy
- Multiple sclerosis
- Stroke
- Alzheimer’s disease
- Parkinson’s disease
- Rheumatoid arthritis
Do not dismiss depression as a normal part of having a chronic illness. Effective treatment for depression is available and can help even if you have another medical illness or condition. If you or a loved one think you have depression, it is important to tell your health care provider and explore treatment options.
Although both chronic disease and mental health disorders are common, strategies exist that can prevent or effectively treat the conditions. Modifiable risk behaviours (i.e., tobacco use, physical inactivity, and poor nutrition) that contribute to a number of chronic diseases and mental health disorders can be targeted. It is never too late to address both individual risk factors and environmental risk factors.
Looking for the best Counselling has to offer? Get Advice!
Common stresses of chronic illness
Chronic or long-term illness and its treatment pose special problems. You need to learn how to:
- live with the physical effects of the illness
- deal with the treatments
- make sure there is clear communication with doctors
- maintain emotional balance to cope with negative feelings
- maintain confidence and a positive self-image.
Ways to cope with chronic illness
There is a range of ways to deal with the stress of chronic illness. These include:
- finding information – this can help if you feel helpless or out of control
- emotional support from others – particularly family and friends. Talk to someone you trust — you don’t have to go through this alone.
- joining a well facilitated support group, social media support groups, online etc.
- setting concrete, short-term goals – to restore certainty, power and control
- thinking about possible outcomes – discussing them with the doctor can help you to face them before they become a reality.
“The overall aim of therapeutic strategies is to help put your illness into context and give some meaning to what is happening”.
It can be difficult to know what to do and how to cope, but help is available. For those that need treatment for more serious disease, seek professional therapy, use medications, self-help measures, go to your doctor and/or emergency care, seek EAP services through work programs, and find community support programs. Lifeskills Australia can help you. Call us today to make an appointment to talk with one of our friendly staff about your next step on your road to recovery.
Where to go to for support?
- Contact Lifeskills: 1800 870 080 (available 24/7)
- Get professional support — contact a helpline, your GP, a counsellor, psychologist or psychiatrist, a hospital emergency department, minister, teacher or anyone you trust to keep you safe.
- If your life is in danger – call emergency services 000